Outpatient Care Initiative
To improve quality of outpatient consultations in MSF projects
The Outpatient Care (OPD) Initiative aims at strengthening the competencies and skills of consultations providers in patient assessment, clinical reasoning and clinical decision-making, using a person-centered model of care, with the goal of improving the quality of outpatient consultations in MSF projects.
Outpatient care is the most common medical service provided by MSF. Outpatient consultations are conducted by a wide variety of health workers, not all with the same training in diagnostics or treatment, depending on the resources at hand. The limited availability of medical doctors in certain low-income countries and gaps in clinical supervision pose challenges in terms of quality of care and clinical decision-making.
The programme is based on a transversal competency framework that was developed based on the key elements of a primary care consultation and the main aspects for improvement identified following a feasibility study and a consultancy between MSF and the Institute of Tropical Medicine in Antwerp, Belgium.

The Outpatient Care initiative in numbers
graduated
we have projects
following the programme
The programme is currently being implemented in Sierra Leone, South Sudan and Nigeria. The programme was successfully completed in Guinea across five health centres along the Kouroussa prefecture from June 2021 to October 2022.
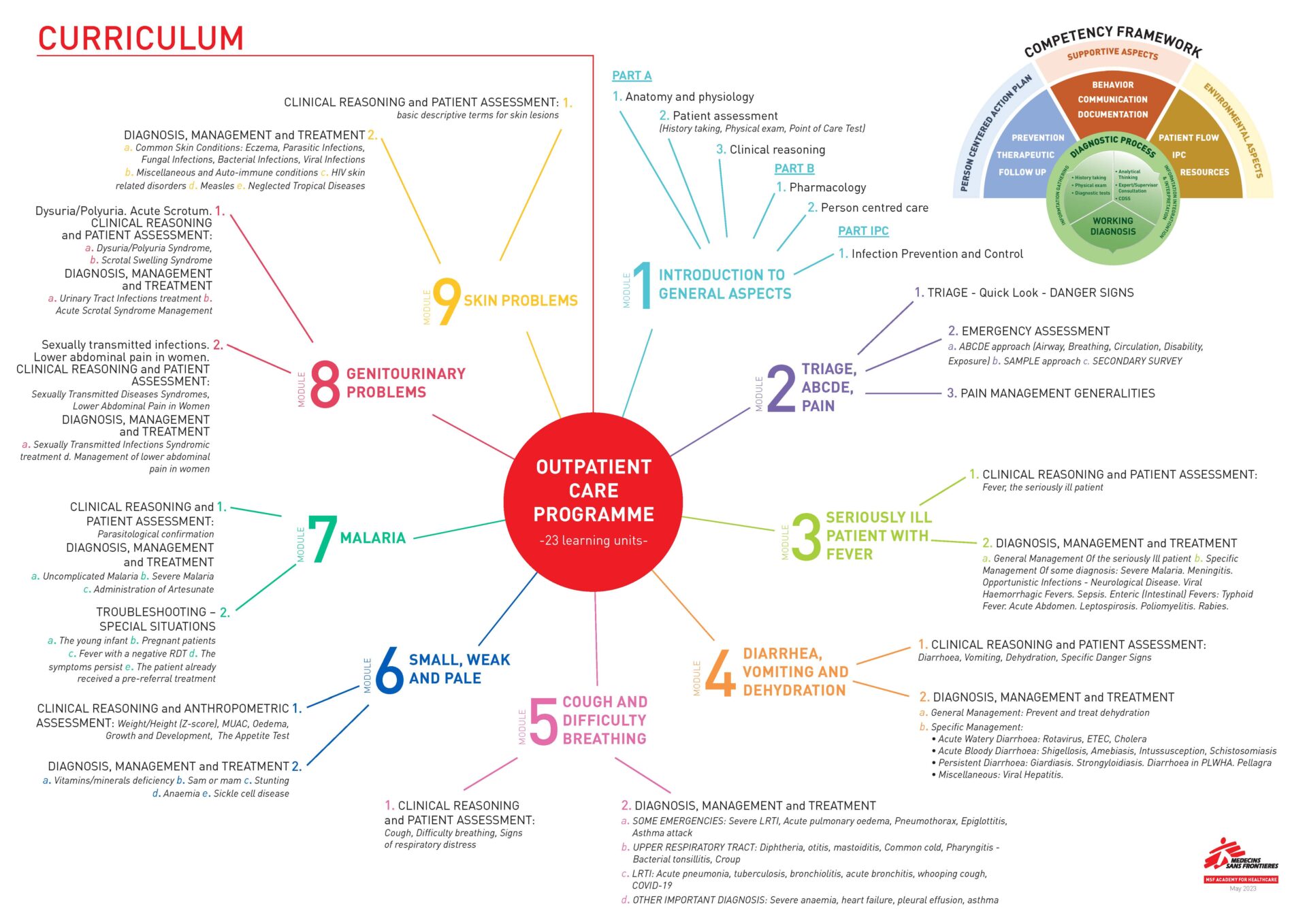
The OPD curriculum
The curriculum is composed of 9 syndromic-based learning modules that relate to the most common situations faced in Primary Care:
Module 1: Introduction to general aspects
Module 2: Triage, ABCDE, pain
Module 3: Seriously ill patient with fever
Module 4: Diarrhea, vomiting and dehydration
Module 5: Cough and difficulty breathing
Module 6: Small, weak and pale
Module 7: Malaria
Module 8: Genitourinary problems
Module 9: Skin problems

The Outpatient Care programme is delivered at the workplace and is implemented in six months. One of the key components is the clinical mentoring.
The implementation is organised in two phases. The three-month ‘intensive phase’ consists on daily group interactive learning activities facilitated by the clinical mentors at the health centre and individual bedside mentoring sessions during working hours, taking in consideration the health centre dynamics and workload. Afterwards, the three-month ‘continuation phase’ consists of mentoring sessions and continuous professional development activities with the aim of consolidating the competencies developed during the first phase.
Each module of the programme contains specific learning material
- Handout Book, with all the study material.
- Learner's workbook, with homework tasks and sessions' guides.
- Facilitator's book, with a step by step guide for the activities facilitation.
- Session plans, with a quick guide for the preparation and facilitation of the learning activities.
- Simulation scripts, a step by step guide to facilitate simulation scenarios developed specially for this course.
- Extra resources: games, presentations and other resources developed for the learning activities.
 A nurse in a Community Health Centre measuring the arm of a baby using MUAC tape to determine if the child is malnourished, Kenema, Sierra Leone, 2021. ©MSF
A nurse in a Community Health Centre measuring the arm of a baby using MUAC tape to determine if the child is malnourished, Kenema, Sierra Leone, 2021. ©MSF
Assessments and evaluation activities
The Competency Gap Assessment (CGA) is the tool used to measure the learning outcomes of the programme, by comparing its results pre- and post- training. It is composed of a knowledge questionnaire and a more practical part: a direct observation of a consultation using a standardised observation checklist focused on the 12 competencies from the Competency Framework and organised following the person-centered consultation structure.